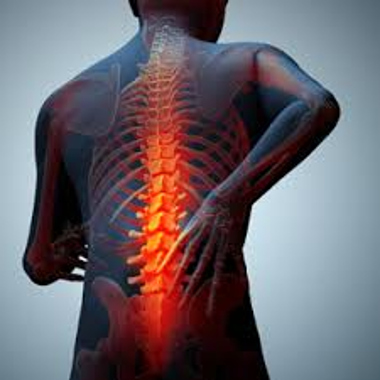
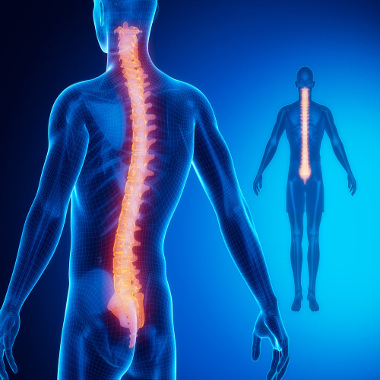
Ankylosing spondylitis is a type of arthritis that affects the spine. Ankylosing spondylitis symptoms include pain and stiffness from the neck down to the lower back.
The spine’s bones (vertebrae) may grow or fuse together, resulting in a rigid spine. These changes may be mild or severe, and may lead to a stooped-over posture. Early diagnosis and treatment helps control pain and stiffness and may reduce or prevent significant deformity.
Who Is Affected by Ankylosing Spondylitis?
Ankylosing spondylitis affects about 0.1% to 0.5% of the adult population. Although it can occur at any age, spondylitis most often strikes men in their teens and 20s. It is less common and generally milder in women and more common in some Native American tribes.
What Are the Symptoms of Ankylosing Spondylitis?
The most common early symptoms of ankylosing spondylitis include:
- Pain and stiffness. Constant pain and stiffness in the low back, buttocks, and hips that continue for more than three months. Spondylitis often starts around the sacroiliac joints, where the sacrum (the lowest major part of the spine) joins the ilium bone of the pelvis in the lower back region.
- Bony fusion. Ankylosing spondylitis can cause an overgrowth of the bones, which may lead to abnormal joining of bones, called “bony fusion.” Fusion affecting bones of the neck, back, or hips may impair a person’s ability to perform routine activities. Fusion of the ribs to the spine or breastbone may limit a person’s ability to expand his or her chest when taking a deep breath.
- Pain in ligaments and tendons. Spondylitis also may affect some of the ligaments and tendons that attach to bones. Tendonitis (inflammation of the tendon) may cause pain and stiffness in the area behind or beneath the heel, such as the Achilles tendon at the back of the ankle.
Ankylosing spondylitis is a systemic disease, which means symptoms may not be limited to the joints. People with the condition also may have fever, fatigue, and loss of appetite. Eye inflammation (redness and pain) occurs in some people with spondylitis. In rare cases, lung and heart problems also may develop.
What Causes Ankylosing Spondylitis?
Although the cause of ankylosing spondylitis is unknown, there is a strong genetic or family link. Most, but not all, people with spondylitis carry a gene called HLA-B27. Although people carrying this gene are more likely to develop spondylitis, it is also found in up to 10% of people who have no signs of the condition.
How Is Ankylosing Spondylitis Diagnosed?
The diagnosis of ankylosing spondylitis is based on several factors, including:
- Symptoms
- Findings of a physical exam
- X-rays of the back and pelvis
- Measurements of the chest when breathing
- Results of lab tests
How Is Ankylosing Spondylitis Treated?
There is no cure for ankylosing spondylitis, but there are treatments that can reduce discomfort and improve function. The goals of treatment are to reduce pain and stiffness, maintain a good posture, prevent deformity, and preserve the ability to perform normal activities. When properly treated, people with ankylosing spondylitis may lead fairly normal lives. Under ideal circumstances, a team approach to treat spondylitis is recommended. Members of the treatment team typically include the patient, doctor, physical therapist, and occupational therapist. In patients with severe deformities, osteotomy and fusion can be done.
- Physical and occupational therapy. Early intervention with physical and occupational therapy is important to maintain function and minimize deformity.
- Exercise. A program of daily exercise helps reduce stiffness, strengthen the muscles around the joints and prevent or minimize the risk of disability. Deep breathing exercises may help keep the chest cage flexible. Swimming is an excellent form of exercise for people with ankylosing spondylitis.
- Medications. Certain drugs help provide relief from pain and stiffness, and allow patients to perform their exercises with minimal discomfort. Nonsteroidal anti-inflammatory drugs (NSAIDs) — such as ibuprofen, naproxen, and aspirin — are the most commonly used drugs for spondylitis treatment. In moderate to severe cases, other drugs may be added to the treatment regimen. Disease-modifying antirheumatic drugs (DMARDs), such as methotrexate, can be used when NSAIDs alone are not enough to reduce the inflammation, stiffness, and pain. In addition, relatively new drugs called biologics — adalimumab (Humira), certolizumab pegol (Cimzia), etanercept (Enbrel), golimumab (Simponi Aria, Simponi), and infliximab (Remicade) — have been FDA-approved for treating ankylosing spondylitis. Also, the antidepressantCymbalta has been approved for chronic back pain as well. Steroid injections into the joint or tendon may be helpful in some cases.
- Surgery. Artificial joint replacement surgery may be a treatment option for some people with advanced joint disease affecting the hips or knees.
How Is Ankylosing Spondylitis Treated?
In addition, people with spondylitis are urged to not smoke or chew tobacco products because smoking aggravates the condition. Certainly, all of the other reasons why doctors discourage smoking also apply here as well.
People with spondylitis are encouraged to sleep on a firm mattress with the back straight. Placing large pillows under the head is discouraged, since it may promote neck fusion in the flexed position. Similarly, propping the legs up on pillows should be avoided because it may lead to hip or knee fusion in the bent position. Choose chairs, tables, and other work surfaces that will help avoid slumping or stooping. Armchairs are preferred over chairs without arms.
Since those with ankylosing spondylitis could easily hurt their rigid necks or backs, special care should be taken to avoid sudden impact, such as jumping or falling.
Source: www.webmd.com
 Robotic Rehabilitation
Robotic Rehabilitation Physiotherapy Rehabilitation Centre
Physiotherapy Rehabilitation Centre Therapeutic horseback riding
Therapeutic horseback riding Hydrotherapy
Hydrotherapy Occupational Therapy
Occupational Therapy Speech Therapy
Speech Therapy Psychological support
Psychological support Isokinetic dynamometry
Isokinetic dynamometry Nutrition & Dietetics
Nutrition & Dietetics Diagnostic units
Diagnostic units Gait Analysis – Foot Pressure Measurement
Gait Analysis – Foot Pressure Measurement Chronic Disease Management Clinic
Chronic Disease Management Clinic Special Outpatient Clinics
Special Outpatient Clinics Social service
Social service